Study: Parents Whose Kids Are Dying Find Out Too Late
Parents of with terminally ill children need information in order to cope, and that is exactly what doctors struggle to give them.
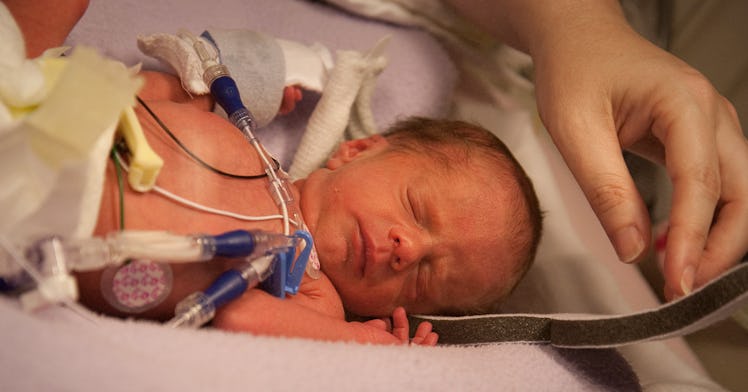
No parent is ever prepared to fully deal with the death of a child, but a new study suggests that they do not have much of a chance to. That is because many doctors wait too long to tell parents that their terminally ill children are running out of time and struggle to communicate other crucial pieces of information about their dying child, according to the findings published in the journal BMJ Supportive & Palliative Care. In fact, nearly half of parents felt they were told their child was out of options all too late. And while better timing and bedside manner will not bring these kids back, improving how healthcare professionals handle these situations could make a world of difference for grieving families.
“Studies have shown that parents who make decisions for their child with advanced cancer consistently indicate the need for truthful and timely delivery of information in non-technical language to build up trust,” oncologist Dr. Camilla Lykke, who co-authored the study, tells Fatherly. “This may help the families to take part in decisions on treatment goals and care on a well-informed basis.”
Playing an active and informed role is incredibly important for the families who have to grieve the loss of approximately 50,000 children in the U.S. every year. For their parents, the death of a child increases the likelihood of divorce and ravages the mental and physical health, making it that much harder for mothers and fathers to survive their late children. One study of over 69,000 women found that their mortality risk shot up 326 percent two years after the death of a child.
And yet, past research indicates that the quality of end-of-life care kids receive — in addition to relieving symptoms and improving quality or even length of life — can help parents cope. It does not change the gravity of their loss, but it is a small but important consolation. It’s also where doctors screw up. Although these situations are excruciatingly difficult for families, research shows that doctors struggle to communicate this sensitive information as well.
To paint an accurate picture of how this affects parents, Lykke and her team surveyed 136 mothers and 57 fathers who had endured the death of a child due to terminal illness — over half of the participating parents’ children did not live past their first year. After parents completed the 122-item questionnaire designed to gauge the perceptions of the quality of communication healthcare professionals offered throughout their child’s treatment up until their death. Results revealed that nearly all parents, 98 percent, agreed that doctors should let moms and dads know as soon as it is clear that their child is out of options.
However, it does not always work out that way, and 42 percent of parents said they were told their child was about to die too late. Even more, 43 percent, said the death came as a shock, suggesting they were not adequately prepared leading up to it, and 31 percent of parents reported that they were not able to say goodbye the way that they wanted. Perhaps even more heartbreaking, 15 percent of parents did not learn their child would die until 24 hours before it happened, 12 percent were not told at all, and 11 percent did not realize their child was dying until they were gone.
“We were quite surprised that 42 percent of the parents answered that none of the attending staff had told them that their child did not have much longer to live,” Lykke said. It’s important to note that the findings are based on parents’ experiences in Denmark hospitals, not U.S. ones, and it’s possible that numbers could be even higher in American hospitals, but that requires further study. Lykke believes the current study is applicable elsewhere.
“This study has been carried out in Denmark, but we believe that our findings could be generic,” she says.
The takeaways for parents with terminally ill children are relatively universal. It’s crucial to make communication expectations clear when children are in palliative clear, especially regarding how and when they want the toughest information, before it gets to that point. What healthcare professionals can learn from this is that handling parents too delicately when their children are dying could break them even more. These parents are already going through one of the hardest experiences imaginable and can handle the truth, but they need to know what to expect and prepare for. And if doctors need additional training or written guidelines in order to tell parents what they need to hear, Lykke recommends that future studies look at the best possible way to do that.
“The results may raise awareness of the importance of providing improved education and training for healthcare professionals working with children with life-limiting diagnoses and their parents,” Lykke added. “In order to improve practice, national guidelines on high-quality end-of-life communication should be considered as a part of the future agenda of specialized pediatric palliative care.”
This article was originally published on