Doctors Just ‘Un-Drowned’ a Child. Here’s How They Did It.
Hyperbaric oxygen therapy is unapproved and untested in drowning victims. So did it really save toddler Eden Carlson's brain after she fell into a swimming pool?
Two-year-old Eden Carlson remained unresponsive. Two months earlier she had hopped over a baby gate and fallen into the family swimming pool, where she remained underwater for 15 minutes before she was discovered and resuscitated. Her prognosis was not good; when she was discharged from the hospital she was alive but immobile, unalert, and unable to communicate. MRI scans showed that the drowning had ravaged her developing brain’s grey and white matter.
In a last-ditch attempt to save Carlson’s oxygen-starved mind, her family travelled to New Orleans for a controversial treatment known as hyperbaric oxygen therapy. According to a new study describing the case—it worked. After 39 HBOT sessions, she regained almost all of her speech, cognition, and movement. Merely five months after drowning, Carlson’s MRI revealed only mild, residual brain damage. “The startling regrowth of tissue in this case occurred because we were able to intervene early in a growing child, before long-term tissue degeneration,” announced case study coauthor Dr. Paul Harch, director of hyperbaric medicine at Louisiana State University School of Medicine, in a statement. “Such low-risk medical treatment may have a profound effect on recovery of function in similar patients who are neurologically devastated by drowning.”
A tragedy was averted–reversed really–but a question lingers even as Carlson returns to her life: Does the case represent a massive breakthrough for HBOT treatments or was it a fluke? A single case study does not represent proof of concept for a treatment plan that remains unapproved and largely untested on human drowning victims. The news is good, but this may not be a mass-market miracle.
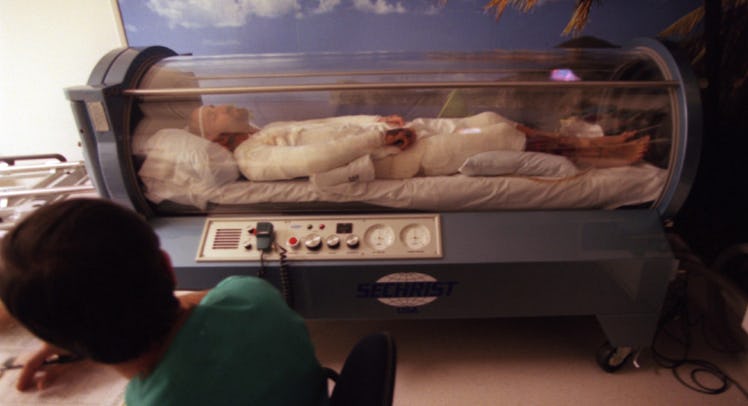
Hyperbaric oxygen therapy involves increasing the air pressure in the room while administering oxygen therapy. Patients either lie down on a table that slides into a plastic tube or sit with their heads in a plastic hood, breathing oxygen through a mask. Therapists then increase the atmospheric pressure inside the tube or hood until it’s roughly three times higher than normal air pressure, and administer oxygen under these high-pressure conditions for about two hours.
Henry’s Law states that the amount of gas that dissolves in a liquid is directly proportional to the partial pressure of that gas, and one outcome of that nifty rule is that higher pressure means more oxygen molecules make it into the plasma. Studies suggest hyperbaric conditions increase the oxygen delivered to a patient 2,000-fold. For oxygen-starved brains, full of idling and dead neurons surrounded by glial cells, it is believed that such high levels of oxygen can shock the brain cells back into action.
It seems to work in animals. Scientists have raided pet stores to test HBOT in rabbits (the study demonstrated that HBOT is safe), cats (found that it repaired damaged brains), and dogs (suggested that it can increase survival rates). Preliminary human studies—almost invariably flawed—have also shown some promise. Which may be why FDA and Medicare approve of HBOT for certain conditions (gas poisoning, specific infections, “the bends”) but stress that it is not approved as a treatment for cerebral palsy, autism, multiple sclerosis, or heart attack. This, despite the fact that many for-profit HBOT clinics advertise “cures” for these very conditions.
Which brings us to drownings and near-drownings. There is little compelling evidence the HBOT helps—Carlson “miracle” aside—and ample evidence that it could harm. Although there has never been a documented fatality due to HBOT, studies have shown that the therapy can lower blood sugar and cause nearsightedness and anxiety attacks. In serious cases, physicians suspect the therapy could collapse a lung or cause seizures due to an oxygen overload. Seriously complications have been reported.
In fact, the risks are so apparent and the rewards so unclear that intensivists famously refused to allow parents of a two-year-old boy who drowned in Florida to try HBOT. The boy’s father argued his case in court, and a circuit court judge ruled in his favor, provided the parents paid for the therapy out-of-pocket and released their physicians from any liability. The child ultimately recovered. Later, however, medical ethicists concluded that the ruling was not necessarily ethical.
“The physician has an independent obligation to act in the best interests of the child,” wrote three ethicists in the Journal of Perinatology. “That obligation is not ended with the ‘informed consent’ of a parent to utilize an unproven or unconventional therapy. Nor does a waiver of liability or a court’s authorization for a procedure absolve the treating physician—so long as there is a realistic opportunity of benefit or protection against harm—from the commitment to act as an advocate for the patient’s well-being.”
So was Carlson saved by hyperbaric oxygen therapy? Even Harch, the physician who administered the therapy, wrote the study, and runs an HBOT clinic isn’t sure. In the case study itself, he writes that Carlson was also given regular oxygen therapy and that it is impossible to rule out that this alone repaired her brain. The Carlson case is a victory for a controversial therapy, and likely to boost interest in HBOT both for its approved and unapproved uses. But from a scientific perspective, it’s still entirely unclear whether HBOT is safe or effective when it comes to drowning victims.
Carlson’s recovery is great news, but may not have broader ramifications for parents. Drowning remains a clear and present danger.
This article was originally published on