Does An Epidural Hurt? And 7 Other Things You Should Know About Epidurals
Hotly debated and frequently misrepresented, here are just the facts about epidurals.
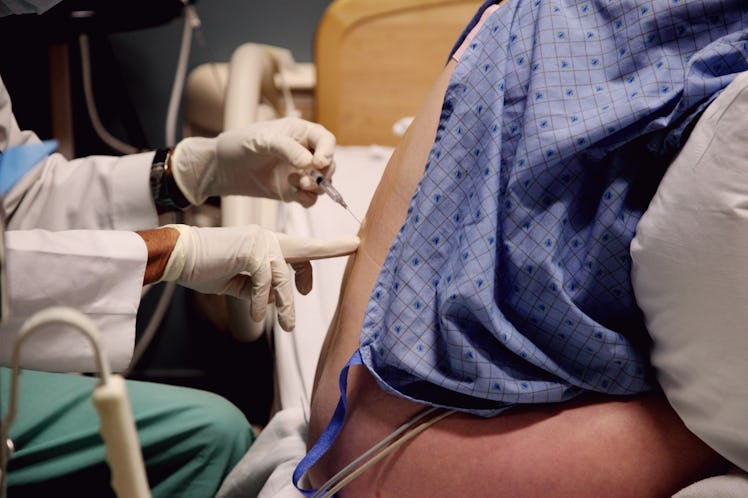
Perhaps no other variable of the childbirth experience is as hotly debated and frequently misrepresented as epidurals. Yes, epidurals take away the pain; but they also raise concerns about the safety of mother and child. Increasingly, though, couples are opting for the procedure during labor: More than half of childbirths today involve using a regional anesthetic to numb the body from the waist down, easing the discomfort of contractions.
“From the perspective of what’s most helpful for women during labor, there’s no question that epidurals ease the pain,” says Raeford Brown, M.D., a professor of anesthesiology and pediatrics at the University of Kentucky Medical Center. Here’s what you should know about the procedure.
1. Epidurals Are Less Painful Than They Look
Getting an epidural hurts about as much as getting an IV. That is to say, your partner will feel a sting or discomfort for a few seconds after the needle is inserted before it diminishes; the actual numbing kicks in after about 20 minutes.
There are actually two needles: The first is for a local anesthetic that numbs the area where the epidural will be placed. The second is a larger needle that leads the catheter into the epidural space. The area should be relatively numb by that point, so the discomfort is minimal.
2. Epidurals Are Not Dangerous
Despite what you may have heard, an epidural does not harm your baby. “The short answer is that there are no proven adverse direct effects on the fetus/newborn,” says pediatrician James J. Cummings, M.D., former chairman of the American Academy of Pediatrics Committee on Fetus and Newborn. “However, there are potential indirect effects, as it may increase the risk for instrumented delivery (using forceps) or operative delivery (C-section) because of failure to progress in labor.”
3. Epidurals Go Near, Not In, The Spinal Cord
Relax, no one is going to be jamming a needle into your partner’s spine. “The spinal cord is surrounded by fibrous elements which in turn are wrapped around a bag-like structure holding water,” says Brown. “There is a space between the bag and the fibrous elements, and this is where the needle goes.” Once this area is desensitized, the labor can proceed pain-free.
4. Not Everyone Should Get An Epidural
Although epidurals are safe for the vast majority of moms-to-be, for a small segment of the population, the procedure is risky. “Women with hypertension that is associated with pregnancy — known as pre-eclampsia — have a problem with the coagulation of their blood,” says Brown. “Within that group, there is an even smaller subset who experience a dropping platelet count, and for these women, epidurals are not advisable.”
5. An Epidural Could Slightly Slow The Labor
Studies suggest how far along a person is in labor can impact whether the epidural slows things down. If given before 5 cm dilation, chances of a slower labor are higher. On the other hand, if contraction pain causes your partner to tense their muscles, labor will take a lot longer, too.
Regardless, because your partner is numb, they won’t necessarily know when to push during a contraction. Not to fear, delivery room doctors and nurses do this all day long. They will guide both of you through the process determined by dilation.
6. Your Partner May Need A Catheter To Pee
Because your partner will be number from the waist down, if they need to urinate during the labor process, they may not get the signals they normally would, resulting in an accident. For this reason, the doctor may place a catheter to help keep the bladder empty.
7. There Is More Than One Type Of Epidural
Two of the most common types of epidurals are continuous infusion, in which a catheter continuously feeds the anesthetic into the body, and a walking epidural, so-called because an injection of painkillers allows the pregnant person limited mobility in their lower limbs. (Note: This does not mean you and your partner can take a brisk stroll around the hospital hallways, but it does mean they may be able to go to the bathroom on their own.)
8. Back Pain From Epidurals Is A Myth
Although there are risks associated with epidurals — including a drop in blood pressure, an increase in the odds of needing forceps for delivery, breathing difficulties, and fever — long-term back pain is not one of them.
“I’ve heard some women say, ‘Now I have back pain because I got an epidural,’” says Brown. “I tell them, ‘No, you have back pain because you just had a baby!’”
In truth, any lower back discomfort after delivery is less likely to have been caused by the anesthesia and more likely to be the result of the very physical activity of labor.
Of course, whether or your partner chooses an epidural is a personal decision. But rest assured that from a safety perspective, the procedure is routine and something your hospital staff is accustomed to performing all day long.
This article was originally published on