Does The HPV Vaccine Help If You’re Already Infected?
Most adults over 26 shouldn’t get the HPV vaccine — but there are exceptions.
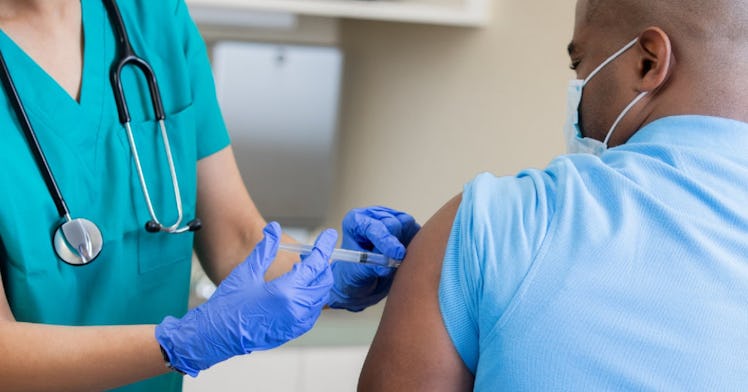
Parents today have the option to protect their kids from cancer with just two quick jabs. The HPV vaccine prevents nine different strains of human papillomavirus, or HPV, a sexually transmitted disease that can cause a range of different cancers, from cervical to penile. Since the vaccine’s approval in 2006, rates of cervical cancer, the fourth most common cancer in women, have steadily dropped. Today, the Centers for Disease Control and Prevention (CDC) recommends that all kids between 11 and 12 years of age receive the HPV vaccine — or anyone as old as 26 who is not already vaccinated. But what about the HPV vaccine for adults past their mid-20s? Is there a hard and fast HPV vaccine age limit? Does the HPV vaccine help if you’re already infected?
For most adults, the HPV vaccine won’t have much benefit — but there are exceptions.
HPV Vaccine For Adults
There are a few reasons why the CDC doesn’t recommend the HPV vaccine to adults older than 26. First, the vaccine simply isn’t as effective in older people, says Lois Ramondetta, M.D., a gynecological oncologist at the University of Texas MD Anderson Cancer Center. “We believe [younger people’s] immune systems are just more robust,” she says. In other words, their bodies pump out more antibodies in response to the vaccine.
But more important is the likelihood of previous exposure to HPV, Ramondetta says. Let’s be frank: If you’re past your mid 20s and unvaccinated, there’s a good chance you’ve already had HPV. “It’s just a part of being human,” Ramondetta says. “Eighty percent of us are going to be exposed at some point.”
Does The HPV Vaccine Help If You’re Already Infected?
The HPV vaccine can’t treat an active infection, and it doesn’t prevent a previous infection from causing cancer down the line, so it’s the most useful in people who haven’t had any previous exposures, Ramondetta says. However, it is possible to gain some protection from the vaccine even if you have been exposed to HPV.
“Just because you’ve been exposed to one of the types of HPV doesn’t mean that the vaccine wouldn’t be useful for you,” Ramondetta says. There are 100 strains of HPV, and 14 are known to cause cancer. Even if you’ve been exposed to one cancer-causing strain, the HPV vaccine, which protects against nine strains, could prevent you from becoming infected with a different one.
Still, the higher your likelihood of previous exposures — meaning the more sexual partners you’ve had and whether you were monogamous — the less useful the vaccine is going to be.
Who Should Get the HPV Vaccine After 26?
Adults who would benefit the most from getting the HPV vaccine include those who haven’t yet been sexually active and those who have been in a monogamous relationship for most of their adult life, Ramondetta says. If this sounds like you, she suggests speaking with a doctor about your options.
But even if those descriptions don’t fit, you can become an advocate for vaccination, Ramondetta says: “Get your kids vaccinated, get your nieces and nephews vaccinated, talk to your friends. Many of our cancers, we just don’t have a clue about how to stop them. But this, we do.”
This article was originally published on